Pelvic Pain
Pelvic pain can be a hallmark symptom of both endometriosis and adenomyosis—often chronic, often cyclical, and sometimes severe enough to disrupt work, relationships, sleep, and daily functioning. Understanding the “why” behind pelvic pain is the first step toward targeted treatment and lasting relief.
Overview
Pelvic pain is pain felt anywhere in the lower abdomen/pelvis—often described as aching, cramping, pressure, stabbing, or burning. In people with suspected or known endometriosis, pelvic pain may be cyclical (worse around periods or ovulation) or persistent throughout the month. With adenomyosis, pain is commonly strongest during menstruation and may occur alongside heavy bleeding and a “boggy” or enlarged uterus.
In endometriosis, endometrial-like tissue can grow outside the uterus (for example on the ovaries, pelvic sidewalls, bowel, bladder, or behind the uterus). These implants can trigger inflammation, scarring, and adhesions that restrict normal organ movement and irritate nearby nerves—creating pain that can flare with hormonal shifts and sometimes persist even between cycles. In adenomyosis, endometrial tissue grows into the uterine muscle, which can cause the uterus to contract more painfully and contribute to deep, heavy cramping and pelvic pressure.
Pelvic pain can overlap with other conditions, which is one reason endometriosis often takes years to diagnose. Symptoms may mimic IBS, bladder pain syndrome/interstitial cystitis, pelvic floor dysfunction, fibroids, or musculoskeletal issues. A key clue is a pattern of cyclical flares, pain with sex, bowel movements, urination, or worsening pain despite “normal” routine testing—but any pattern deserves a thoughtful evaluation. A specialist-led workup through an experienced team can help identify endometriosis and common look‑alikes or coexisting issues (see Evaluation & Diagnosis and Related Conditions).
Living with chronic pelvic pain can be isolating and exhausting. It may affect concentration, physical activity, intimacy, mood, and confidence in your body—especially when pain is minimized or mislabeled as “normal period pain.” You deserve to be taken seriously, and effective care is possible with a plan that addresses both symptom relief and root causes.
What It Feels Like
Pelvic pain can feel different from person to person—even among people with the same diagnosis. Many describe a deep, low ache or heaviness in the pelvis, cramping that feels “labor-like,” sharp stabbing pains, or a pulling sensation that worsens with movement, bowel movements, urination, or intercourse. Some people notice pressure in the rectum or vagina, or pain that radiates into the lower back, hips, or thighs.
A common endometriosis pattern is flares that intensify in the days leading up to a period and during bleeding, but pain can also spike mid‑cycle (around ovulation) or after physical activity. With adenomyosis, pain is often centered in the uterus—deep, intense menstrual cramps and pelvic tenderness—and may be accompanied by a feeling of pelvic fullness or bloating.
Over time, persistent inflammation and nerve sensitization can make pain less tied to the cycle and more constant. Some people develop “good days and bad days,” where stress, sleep loss, certain foods, or pelvic floor muscle tension amplify symptoms. If your pain is escalating, spreading, or becoming less predictable, that’s a sign you may need a more comprehensive evaluation and a multi‑layer treatment approach.
How Common Is It?
Pelvic pain is one of the most common reasons people seek evaluation for endometriosis. Endometriosis affects about 10% of women of reproductive age, and chronic pelvic pain is a frequent presenting complaint—though the exact proportion varies by study and by how pelvic pain is defined.
In adenomyosis, pelvic pain—especially severe period pain—is also common, often alongside heavy menstrual bleeding. Many people have both adenomyosis and endometriosis, which can intensify pain and broaden symptom patterns (uterine cramping plus pain from lesions/adhesions elsewhere in the pelvis).
Importantly, pain severity does not reliably match “stage” or how much disease is seen on imaging or at surgery. Some people have extensive disease with modest pain, while others have severe pain with minimal visible lesions—especially when deep disease, adhesions, pelvic floor dysfunction, or nerve involvement are present.
Causes & Contributing Factors
In endometriosis, pelvic pain is driven by a combination of inflammation, scarring, and nerve involvement. Endometrial-like tissue outside the uterus can bleed and inflame surrounding structures, releasing inflammatory chemicals that irritate nerves and increase pain sensitivity. Over time, the body may form adhesions (scar tissue bands) that tether organs, making normal movement—like bowel filling, bladder emptying, or intercourse—painful.
Deep infiltrating endometriosis can involve tissues rich in nerves and create pain with specific functions (for example, bowel movements or urination). Endometriomas (ovarian cysts associated with endometriosis) can contribute to aching or sharp pain, especially with activity or around the cycle.
In adenomyosis, endometrial glands within the uterine muscle can lead to thicker, more reactive uterine tissue and stronger uterine contractions during menstruation. This can cause intense cramping, pelvic pressure, and tenderness. Adenomyosis-related inflammation may also amplify pain signaling and contribute to fatigue.
Other factors can worsen pelvic pain even when the underlying disease is stable: pelvic floor muscle spasm/guarding, central sensitization (a “wound-up” nervous system), coexisting bladder or bowel conditions, and stress-related changes in pain processing. That’s why many patients benefit most from a plan that addresses both the disease and the pain system (see Pain Management).
Treatment Options
Treatment for pelvic pain usually works best when it targets both symptom control now and long-term drivers (endometriosis lesions, adenomyosis, adhesions, and nervous system sensitization). Options are individualized based on your goals (pain relief, fertility, avoiding hormones, avoiding hysterectomy), severity, and whether adenomyosis and endometriosis coexist.
Medical options may include anti-inflammatory medications (like NSAIDs), nerve-pain–targeted medications for neuropathic components, and hormonal suppression to reduce cyclical inflammation and bleeding. Hormonal approaches (such as continuous birth control, progestins, or other suppressive therapies) can reduce flares for some patients, though they don’t remove endometriosis tissue and may not be tolerated by everyone. Learn more about medication approaches in Hormonal Therapy and symptom-focused care in Pain Management.
Surgical treatment is often considered when pain is persistent, progressive, or not responding to medical management—or when imaging/exam suggests deep disease, endometriomas, or significant adhesions. For endometriosis, excision surgery (removing lesions at the root) is widely regarded as the gold standard because it aims to remove disease rather than burn the surface. At Lotus, advanced minimally invasive approaches are central to care; explore Surgery & Advanced Excision and learn about surgeon expertise with Dr. Steven Vasilev. Adenomyosis treatment may range from hormonal therapy and uterine-sparing options to hysterectomy in select cases, depending on symptoms and fertility goals (see adenomyosis).
Pelvic floor physical therapy can be a game-changer when muscles tighten in response to chronic pain (a common, treatable pain amplifier). Therapy may focus on down-training/relaxation, trigger point release, breathing mechanics, and gentle strengthening—often improving pain with sex, bowel movements, and daily activity (see Pelvic Floor PT and Pelvic Floor Dysfunction).
Lifestyle and integrative supports can complement medical/surgical care: heat, TENS, pacing and flare plans, anti-inflammatory nutrition strategies, sleep support, stress reduction, and selected supplements when appropriate. These tools won’t “cure” endometriosis or adenomyosis, but they can reduce suffering and improve function while you pursue definitive diagnosis and treatment (see Integrative Medicine & Lifestyle Care and At-Home Remedies). What to expect: meaningful improvement is possible, but it may take a layered plan and time—especially if pain has been present for years.
When to Seek Help
Seek urgent care immediately if pelvic pain is sudden and severe (especially one-sided), accompanied by fainting, shoulder pain with dizziness, fever, persistent vomiting, heavy bleeding soaking pads hourly, black/tarry stools, blood in urine, or if you could be pregnant (to rule out ectopic pregnancy or other emergencies). Also seek urgent evaluation for new neurologic symptoms (leg weakness/numbness) or inability to pass urine.
Schedule a specialist evaluation if pelvic pain is chronic (most days for 3+ months), repeatedly causes missed school/work, worsens around your period, or occurs with sex, bowel movements, urination, or infertility concerns. If you’ve been told imaging is “normal” but your symptoms persist, that does not rule out endometriosis—many cases require expert assessment and, when appropriate, surgical diagnosis.
To make your visit more effective, bring a symptom timeline (cycle days, triggers, bowel/bladder symptoms, medications tried, and functional impact). If you’re ready for a deeper evaluation and a clear plan, you can schedule a consultation with Lotus. Our team focuses on thoughtful diagnosis and individualized care for both endometriosis and adenomyosis (see Evaluation & Diagnosis).
Frequently Asked Questions
How rare is endosalpingiosis?
Endosalpingiosis is generally considered uncommon, but “how rare” it is depends heavily on who’s being studied and how it’s found. Many cases are discovered incidentally on pathology—meaning tissue is identified under the microscope after surgery done for other reasons—so it’s likely underrecognized in the general population. In other settings (like surgical cohorts), it may appear more often simply because more tissue is being sampled and examined carefully.
What matters most for patients is that endosalpingiosis can be confused with endometriosis on imaging or even at surgery, yet it doesn’t always behave the same way clinically. If you’ve been told you have endosalpingiosis and you also have pelvic pain, bowel/bladder symptoms, or fertility concerns, our team can help interpret what that finding means in the context of your symptoms and operative/pathology reports. You’re welcome to explore our educational content on related endometriosis and uterine conditions, and reach out to schedule a consultation if you want a personalized plan.
Can endometriosis cause a painful bump near the anus?
Yes. Endometriosis can contribute to pain and pressure around the rectum and anal area, especially when disease involves the rectum/rectosigmoid region or nearby tissues. Many patients describe deep pain with bowel movements, rectal pressure, or symptoms that flare around their cycle, and those patterns can fit bowel or deep infiltrating endometriosis.
That said, a sensitive bump on the anus itself is more often something else (like a hemorrhoid, fissure, skin infection/abscess, or another localized anal/skin condition). In some cases, pelvic disease can coexist with these issues, which is why we don’t assume every finding is endometriosis—or dismiss it as “nothing.”
If you’re noticing a new, persistent, or worsening bump—especially if it’s very tender, draining, bleeding, or associated with fever—we want to evaluate the full picture. Our team can sort out whether your symptoms point toward bowel endometriosis, a separate anorectal condition, or both, and plan next steps such as a focused exam and, when appropriate, expertly interpreted imaging to map possible deep disease.
What is the AAGL endometriosis classification system?
The AAGL endometriosis classification system is a standardized way surgeons describe what they found at surgery—where endometriosis is located, how extensive it is, and how complex the disease appears. Its goal is to create a more consistent “shared language” than older staging alone, especially for cases where symptoms and imaging don’t tell the full story.
Unlike simple stage labels, AAGL-style classification is meant to better capture real-world surgical complexity, including deeper disease that can involve structures like the uterosacral ligaments, rectovaginal space, bowel, bladder, or ureters. This matters because location and depth (for example, deep infiltrating disease) can drive very different symptoms and may change imaging choices and surgical planning. If you’re reading an operative report or trying to make sense of what a surgeon told you, our team can help translate the classification into what it likely means for your body, your symptoms, and the treatment path you’re considering.
What is pelvic dissection in endometriosis surgery?
Pelvic dissection in endometriosis surgery means carefully separating and opening tissue planes in the pelvis so we can clearly see normal anatomy and remove disease safely. Endometriosis can cause inflammation and scarring that “glues” organs together (sometimes called a frozen pelvis), so dissection is often the step where we free adhesions and restore normal relationships between the uterus, ovaries, bowel, bladder, and pelvic sidewalls.
In practical terms, pelvic dissection may include identifying and protecting critical structures like the ureters, bladder, bowel, blood vessels, and pelvic nerves before excising endometriosis at its roots. This is where surgical precision matters: the goal is to fully address disease while minimizing injury to healthy tissue, especially in complex or re-operative cases. If you’re seeing this term on an op note or surgical plan, it usually reflects the complexity of the anatomy and the deliberate work needed to make excision both complete and safe—our team can walk you through exactly what was dissected and why in your specific case.
When is menstrual bleeding considered too heavy?
Menstrual flow is generally “too heavy” when it consistently disrupts your life or overwhelms your usual period products—think flooding or soaking through pads/tampons quickly, passing frequent or large clots, needing to double up, or bleeding long enough that you can’t plan around it. Another major clue is fatigue, dizziness, or shortness of breath that can come with iron deficiency from ongoing blood loss. If you’re timing your day around bathrooms, waking at night to change products, or avoiding work, exercise, travel, or sex because of bleeding, that’s not something we consider “normal.”
Heavy bleeding is a symptom, not a diagnosis, and common underlying drivers include adenomyosis, fibroids, hormonal imbalance, and sometimes endometriosis—especially when heavy bleeding shows up with severe cramps or deep pelvic pain. Because imaging and symptoms don’t always match (a scan can look “mild” while symptoms are intense), we take a symptom-led approach and look at the full pattern, including pain, pressure, clots, cycle timing, and any signs of anemia. If your bleeding feels like it’s escalating or you’ve been told to “just live with it,” our team can help you sort out likely causes and build a plan that targets the source—not just the bleeding.
Can endometriosis cause arthritis-like joint pain?
Yes—endometriosis can be associated with arthritis-like joint pain in some people, even though joint pain isn’t considered a classic “core” symptom. Endometriosis can drive chronic inflammation and immune dysregulation, and that whole-body inflammatory state may show up as aching, stiffness, or flares that feel similar to inflammatory arthritis. Some patients also notice joint symptoms that cycle with their period or worsen during broader endometriosis flares.
At the same time, endometriosis doesn’t “equal” autoimmune arthritis, and an association doesn’t prove that one causes the other. Research suggests higher rates of certain autoimmune conditions in people with endometriosis—including inflammatory diseases that can affect joints—so persistent joint pain deserves a full-picture evaluation rather than being automatically attributed to pelvic disease alone. If you’re dealing with pelvic pain plus joint symptoms, our team can help you sort out what fits endometriosis, what may be a related immune condition, and how that affects your treatment plan, including whether excision surgery and coordinated integrative support make sense for you.
How does estrogen affect the endometrium?
Estrogen is one of the main hormones that drives endometrial growth. In the first half of the menstrual cycle, rising estrogen signals the endometrium to thicken and rebuild after a period, preparing the uterus for a possible pregnancy. It also influences the local immune and inflammatory environment in the uterus, which is part of why hormonal shifts can change bleeding patterns and pain.
When estrogen’s growth signals are strong—and progesterone’s “calming” effect is weaker than expected (often described as progesterone resistance)—the endometrium can behave in a more persistently inflamed, reactive way. This hormone–inflammation pattern is especially relevant in estrogen-dependent conditions like adenomyosis and endometriosis, where tissue similar to the endometrium can contribute to ongoing symptoms. If you’re trying to make sense of heavy bleeding, severe cramping, or cycle-linked pelvic pain, our team can help you connect the hormonal biology to what you’re feeling and review next steps for diagnosis and treatment.
What does advanced adenomyosis mean?
“Advanced adenomyosis” usually means the adenomyosis is more extensive within the uterine muscle—often involving a larger area (diffuse disease), deeper penetration into the myometrium, and/or more pronounced changes like uterine enlargement and tenderness. It’s not the same as “advanced endometriosis,” because adenomyosis doesn’t spread outside the uterus; “advanced” is more about how much of the uterine wall appears affected and how significantly it’s impacting symptoms.
Because adenomyosis doesn’t have a single universally accepted staging system, different clinicians and radiology reports may use “advanced” to summarize imaging features (ultrasound or MRI) and the overall clinical picture—such as heavy bleeding, severe period pain, pelvic pressure, or fertility challenges. In our practice, we focus less on the label and more on what your imaging suggests (diffuse vs focal/adenomyoma, junctional zone changes, uterine size) and what your goals are (pain control, bleeding control, fertility preservation, or definitive treatment). If you’ve been told you have “advanced adenomyosis,” our team can help you interpret what that means in your specific case and map out next steps.
Related Articles
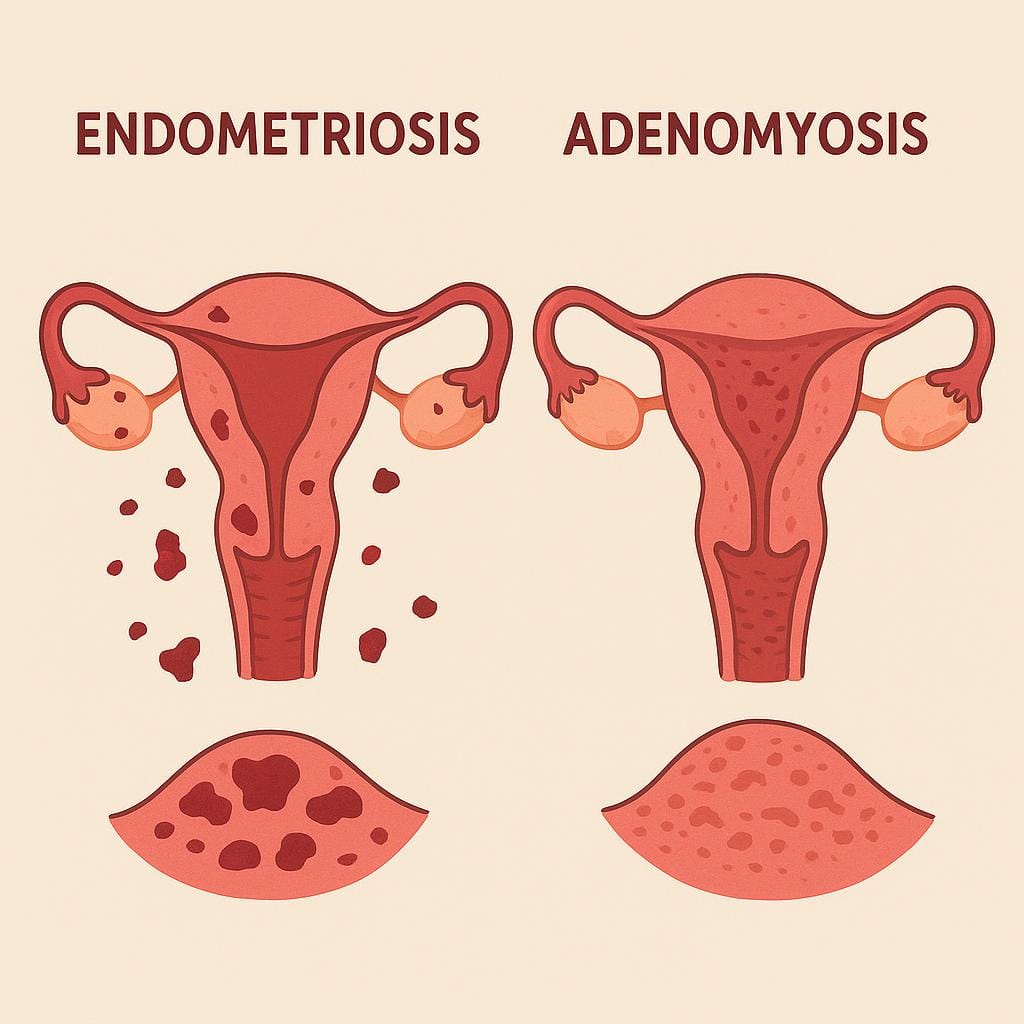
Endometriosis and Adenomyosis: How They Drive Pelvic Pain
Compare endometriosis and adenomyosis: similarities, differences in location and prevalence, diagnosis methods, and treatment options for pelvic pain.

Dienogest vs. Combined Oral Contraceptives for Endometriosis Pain: What a 2025 Meta-Analysis Found
A 2025 meta-analysis of dienogest vs OCPs for endometriosis pain: dienogest helps generalized pain; OCPs help pelvic pain/dyspareunia. Similar side effects.
Different Types of Endometriosis Pain Explained
Explore types of endometriosis pain, evaluation, and evidence-based treatments, including triggers, pelvic floor therapy, CNS sensitization, and adenomyosis.

Post-Orgasm Pain in Endometriosis: Causes and Management
Why orgasms can trigger endometriosis pain: how to ease post-sex discomfort. Causes, symptoms, meds, pelvic floor therapy, surgical options, and sex tips.

Natural Approaches to Managing Endometriosis Pain
Learn how TENS, diet changes, CBD, turmeric, meditation, yoga, and acupuncture can complement care and help relieve pelvic pain from endometriosis.
Experiencing Pelvic Pain?
If you're dealing with this symptom, our specialists can help determine if endometriosis may be the cause and discuss your treatment options.
Schedule a Consultation
